OP is usually treated with corticosteroids. Most often, CT imaging reveals ill-defined patchy consolidation with a predominantly subpleural or peribronchial distribution. Numerous different radiological patterns can be observed and distribution is frequently diffuse or bilateral, although focal or unilateral abnormalities may be present. This form of lung damage can be typically seen as bilateral or unilateral areas of consolidation with patchy distribution in chest radiography however, high-resolution computed tomography (CT) is the gold standard imaging method for the diagnosis of OP. The characteristic histological features of OP include intraluminal organising fibrosis in distal airspaces, with patchy distribution, preservation of lung architecture, uniform temporal appearance, and mild interstitial chronic inflammation. It can be either cryptogenic (COP) when there is no identifiable cause or secondary when it is triggered by infections, medications, or pulmonary/systemic diseases. OP is an anomalous process of pulmonary tissue repair with a characteristic histological pattern of lung damage with radiologic and clinical translation. Since its appearance, several cases of SARS-CoV-2-induced organising pneumonia (OP) have been reported in patients presenting clinical deterioration following an initial period of symptomatic improvement. It was first identified in the city of Wuhan in the Hubei province, China, in December 2019, where it is hypothesised to have emerged. It increases the length of stay, but not all patients require specific treatment and OP may improve despite the absence of high-dose corticosteroid treatment.Ĭoronavirus disease 2019 (COVID-19) is an infectious disease caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). In conclusion, SARS-CoV-2-induced OP may be more frequent than previously thought, especially among hospitalised patients and patients with a more severe disease, particularly those who fail to improve after the second week of disease or who present higher inflammatory markers on admission. Only 38% of OP patients required treatment with high-dose corticosteroids. The use of remdesivir or dexamethasone did not impact the diagnosis of OP. No other differences were identified between OP and controls after adjusting for other factors. 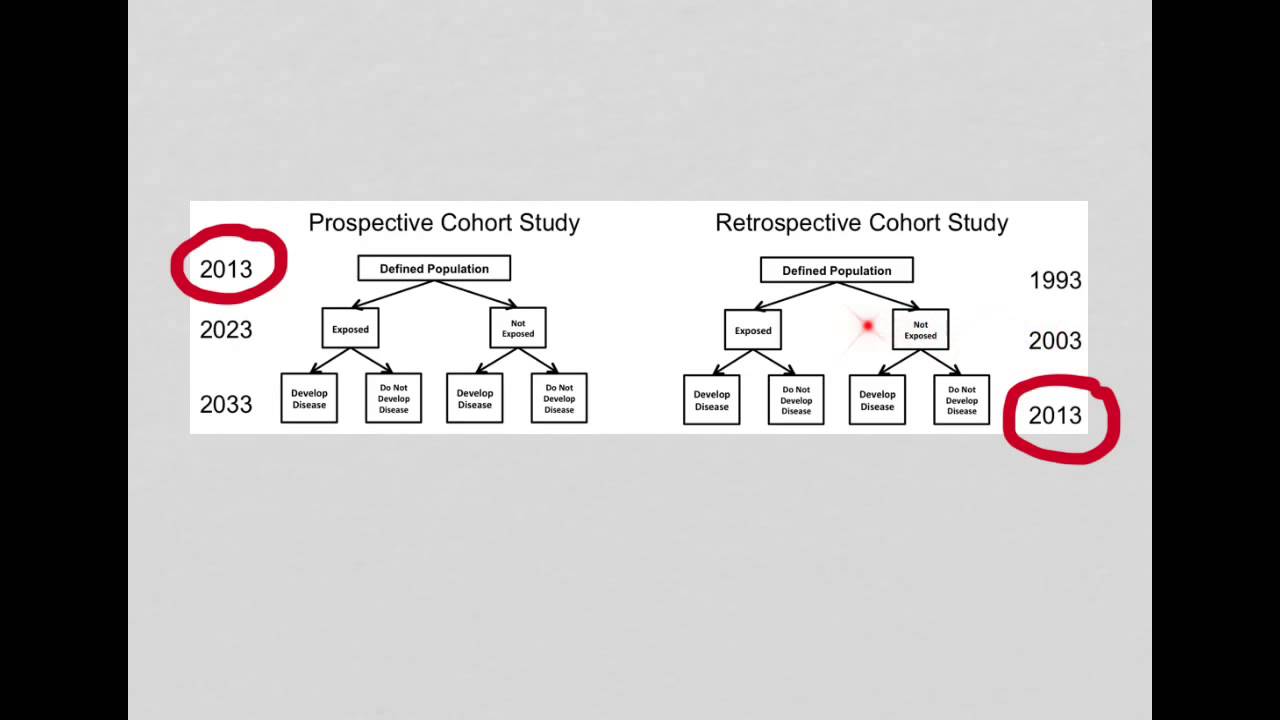
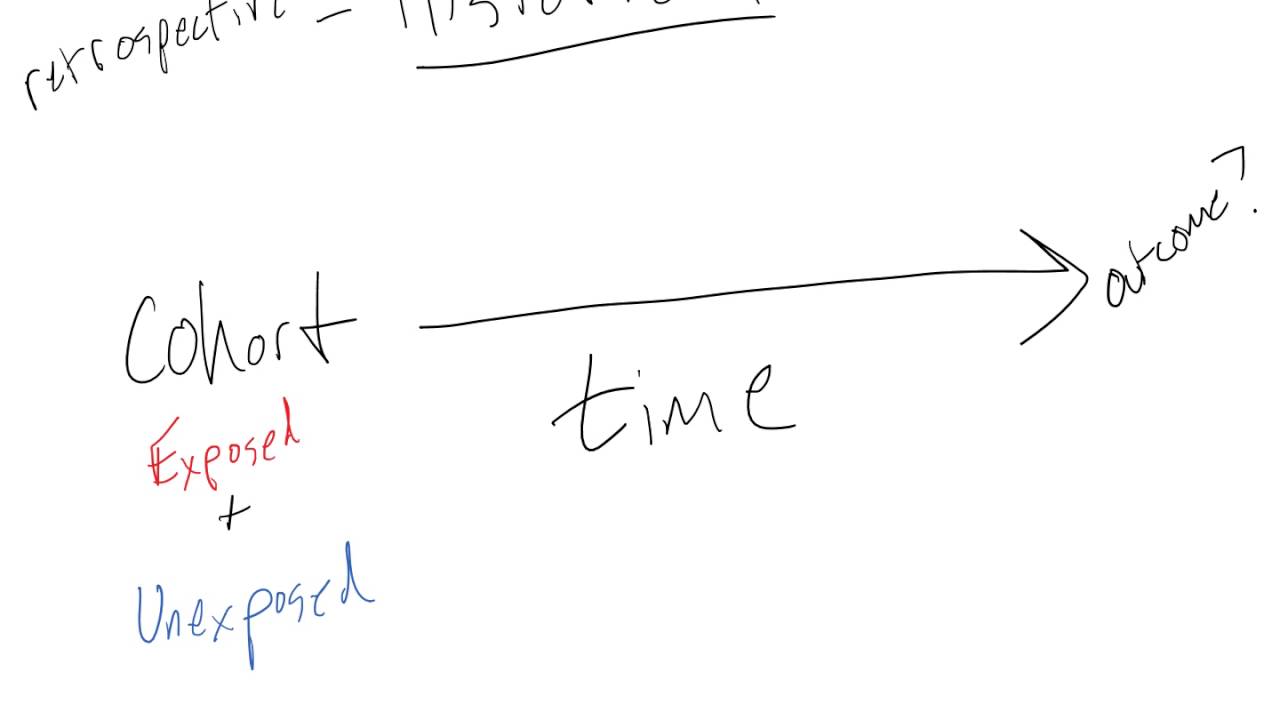
In the adjusted effects model, the need for supplementary oxygen on the 21 st day after symptom onset, the presence of Ordinal Scale for Clinical Improvement (OSCI) = 4, when compared to OSCI ≤ 3, and higher C-reactive protein on admission, were significantly associated with higher odds for OP. OP patients had longer hospitalisation (19.5 vs 10 days, p=0.002) and more frequent ICU admission, but no significant differences in readmittance or mortality rates within 180 days compared to controls. Among OP patients, the most common chest CT-scan findings were consolidations, arciform condensations, and subpleural bands. One hundred fifteen patients were included, of whom 48 (41.7%) fulfilled clinical and imaging criteria for OP. Demographics, comorbidities, disease severity, dexamethasone/remdesivir treatment, laboratory results, and outcomes were compared between groups. We conducted a retrospective case-control study including hospitalised patients due to COVID-19 who performed a chest CT scan during hospitalisation and compared patients with clinical and radiological evidence of OP to patients without evidence of OP. Secondary organising pneumonia (OP) induced by SARS-CoV-2 infection is a recently recognised complication of COVID-19. We aimed to evaluate the prevalence of OP among hospitalised patients with COVID-19 pneumonia and to assess whether disease severity and other clinical factors and comorbidities are correlated with OP development. Coronavirus disease 2019 (COVID-19) is an infectious disease caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
